Hurst NF et al. 2015, Inflamm Allergy Drug Targets
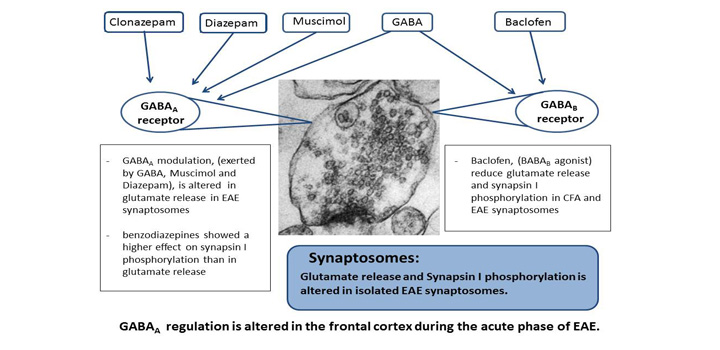
Experimental autoimmune encephalomyelitis (EAE) is an inflammatory demyelinating disease that mimics many of the clinical and pathological features of multiple sclerosis. We have previously described a significant diminution in the GABAergic regulation of glutamate release from synaptosomes of EAE rats isolated during the acute stage of the disease. In order to explore the possible metabolic pathways responsible for this alteration, in this work we evaluate the direct effect of different GABAergic agonists on the glutamate release and concomitant synapsin I phosphorylation in synaptosomes from the frontal cortex of control and EAE animals. The results show that GABA as well as the GABA receptor agonists Muscimol (GABAA agonist) and Baclofen (GABAB agonist) caused a decrease in glutamate release in control rats paralleled by a similar reduction in synapsin I phosphorylation. Meanwhile synaptosomes from EAE animals are responsive only to Baclofen with respect to nontreated EAE synaptosomes, since glutamate release from the synaptosomes treated with Muscimol was similar to that observed in EAE rat synaptosomes which was already reduced as consequence of the disease. In the case of the benzodiazepines Diazepam and Clonazepam (GABAA allosteric agonists), both of them induced a reduction in glutamate release in synaptosomes from the CFA rats, effect that was only observed in synaptosomes of EAE rats treated with Clonazepam. In all cases both benzodiazepines showed a higher effect on synapsin I phosphorylation than in glutamate release. These results indicate that the extent of GABAergic modulation of presynaptic terminals depends on the type of agonist employed and this regulation is altered in the frontal cortex during the acute phase of EAE with respect to control animals.
Autores: Hurst NF, Chanaday NL, Roth GA
Artículo: Hurst NF et al, Inflamm Allergy Drug Targets. 2015 Dec 1.